»
Danh Mục Bài Viết
»
Kỹ thuật phẫu thuật
»
Danh Mục Bài Viết
»
Kỹ thuật phẫu thuật
Laparoscopic Left Colectomy, Including Sigmoid Colectomy( kỹ thuật, cắt đại tràng trái bao gồm cả đại tràng sigma)
Thứ bảy - 25/06/2011 15:08Step 1.
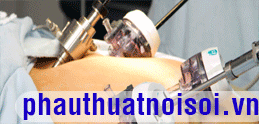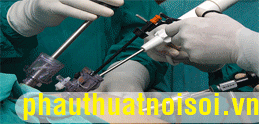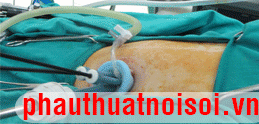
The surgeon begins on the patient’s right (Fig. 1 ). The abdomen is insufflated through an umbilical incision, using a Veress needle. Insert a 5 mm port through the umbilicus, and then a 10-mm port in the right lower quadrant. Starting this way gives the surgeon an idea concerning the anatomy of the left and sigmoid colon and redundancy of the sigmoid; this results in better placement of the GelPort. Some dissection can be done using a Harmonic Scalpel through the 10-mm port in the right lower quadrant. Five-millimeter ports are then placed in the left lower quadrant and right upper quadrant. The GelPort (Fig. 2 ) is placed in an appropriate position as determined by the surgeon, usually suprapubic or low midline.

Figure 1

Figure 2
Step 2.
Changing location, the surgeon now stands on the patient’s left. With the patient in the lithotomy position in steep Trendelenburg, the right side of the mesorectum is taken down using the Harmonic Scalpel. This is facilitated by the surgeon grasping the rectosigmoid and placing traction on it toward the left, thus exposing the right mesorectum. Placing the angled scope in the RLQ or RUQ with the Harmonic Scalpel in the umbilical port should facilitate this dissection. Early dissection of the right mesorectum aids later vascular dissection and is more naturally performed from the left of the patient.
Step 3.
The surgeon moves toward the patient’s right. The patient is still in Trendelenburg but the table is now rotated so that the patient’s right side is down. Grasp the rectosigmoid and retract toward the right to expose the left mesorectum. Using the Harmonic Scalpel, incise the mesorectum. Continue in the left gutter along the white line of Toldt, carrying it all the way up as high as possible to the splenic flexure. This is facilitated by the surgeon placing traction on the sigmoid and left colon and inserting his finger in the avascular plane under the peritoneum in the gutter. The assistant is in charge of both the camera and of maintaining traction of the colon cephalad for dissection along a broad plane to allow easy identification of the left ureter and gonadal vessels.
Step 4.
Mobilize the splenic flexure. This is accomplished best with the surgeon between the patient’s legs using the left hand for traction and the LLQ (or LUQ) port for Harmonic dissection. The patient is still rotated right side down with leveling of the Trendelenburg from full reverse to flat. The assistant grasps the omentum and retracts it cephalad. The surgeon places gentle traction on the left colon and near the splenic flexure. Using the Harmonic Scalpel or laparoscopic Metzenbaum scissors, take down the avascular plane between the omentum and the colon. Again using the Harmonic Scalpel, take down the attachments of the colon to the spleen (splenocolic ligament).
Step 5.
Now the mesentery is ready to be divided. On each side of the lymphovascular structure to be divided, create a window. Insert a 30- or 45-mm endoscopic GIA stapler with vascular loads. The surgeon and the assistant are on the same (right) side of the patient and the stapler can be introduced through the RLQ port. The surgeon’s hand (usually the right, but possibly the left) can be used to safely insert the stapler, protect the bowel, manually control the vessel during stapler placement and after firing and to maintain control of the stump of the vessel in case of bleed-through. Repeat as necessary, working upward toward the transverse mesocolon.
Step 6.
Divide the rectosigmoid by inserting the 60 mm endoscopic GIA through the RLQ port or approach the resection through the hand-port incision by placing a TA 60 mm stapler through the incision.
Step 7.
The sigmoid colon can then be extracted from the protected GelPort incision and transected at an appropriate proximal location and removed from the field. Make the anastomosis with an EEA stapler using the triple-staple technique (see “Low Anterior Resection, Triple-Staple Procedure” described earlier in this chapter).
Step 8.
It is paramount that the surgeon check the doughnuts retrieved from the stapler to make sure they are intact. At this point the pelvis is filled with water and a rigid sigmoidoscope is inserted into the rectum for a short distance to insufflate the colorectal segment; look for bubbles, which would indicate a leak. If a leak is found, it should be repaired and the anastomosis retested. For connections significantly at risk, a diverting colostomy should be considered. Suction out the irrigation fluid. Remove all trocars. Close fascia with a 1 PDS suture. Close skin with a 4–0 Vicryl subcuticular suture.
Tác giả bài viết: Dr. Ai
Những tin mới hơn
Những tin cũ hơn
ĐĂNG NHẬP
CÁC BỆNH THƯỜNG GẶP
- BỆNH THOÁT VỊ BẸN
Tư Vấn Trực Tuyến
Thống kê truy cập
![]() Đang truy cập :
209
Đang truy cập :
209
•Máy chủ tìm kiếm : 43
•Khách viếng thăm : 166
![]() Hôm nay :
18478
Hôm nay :
18478
![]() Tháng hiện tại
: 76120
Tháng hiện tại
: 76120
![]() Tổng lượt truy cập : 47885988
Tổng lượt truy cập : 47885988

 Xem phản hồi
Xem phản hồi Gửi phản hồi
Gửi phản hồi